The First World War saw many advances and adaptations in the field of medicine. As the nature of warfare and types of wound inflicted by new weapons changed, battlefield surgeons adapted. Technologies that had been developing in the years before the conflict grew in importance. Surgical techniques were acquired; imaging techniques improved; skin grafting developed. New problems faced doctors, surgeons and nursing staff. Inhalation of gas saw frontline medicine tested. The attrition of war in the trenches saw shell shock become a problem, one that often was misunderstood by the authorities.
How was first aid and medical service organised on the Western Front?
For the British on the Western Front the system of dealing with the wounded was based around battalions. Each Battalion had a medical officer and was assigned stretcher bearers. A minimum of 16 men were allocated this duty per Battalion. The job of the medical officer at the front line was to establish a first aid post, typically just behind the front lines. From here the wounded were transferred to advanced dressing stations where the field ambulance teams would provide the initial care.

From Advanced Dressing Stations men could then be transported or walked to a more established field hospital or casualty clearing station. Depending on the wounds, treatment could then be carried out at this field hospital, dressings and treatments assessed and administered. This could include surgery. Men could then be moved back to their units if injuries were light, to other hospitals, or sent back to England for treatment in designated hospitals. Dedicated hospital trains and ships were in place to cater for the wounded. Many hospitals on the home front were assigned wounded soldiers and additional hospital space was created by converting larger buildings such as country homes. The Royal Army Medical Corps oversaw all of the medical organisation for the British Army.
Treatment of shrapnel wounds – Gillies and Plastic Surgery
Shrapnel is the name given to the fragments that are sent flying at speed by an explosion. It could be anything from shards of red hot metal to small pieces of stone. In close proximity to an explosion it is the shrapnel that is most likely to cause wounds: any closer and the outcome would most likely be death. Shrapnel causes a huge problem for surgeons. There are many pieces sent flying by an explosion. It travels at speed. This can result in lots of pieces being embedded deep into a wounded soldier. Many shrapnel wounds were to the faces of soldiers, leading to them being disfigured.

The Army employed a New Zealander called Dr. Harold Gillies. He experimented with an early form of plastic surgery. Gillies utilised a method now known as the forehead flap. It took cartilage from the ribs and implanted it into the forehead. This could be moulded over time to reconstruct facial function and features. Gillies, operating out of a specialist hospital at Sidcup, had many successes but also many failures. As his work was experimental and a new method of approaching facial reconstruction he made mistakes. Crucially, he learnt from them and this led to significant improvements in facial reconstruction methods. He learnt to proceed slowly as the body could reject changes or the wound could become infected.
The BBC have a very useful resource on How to fix a face that has been blown off by Shrapnel. It includes visual examples of Gillies work and the limitations of medicine in the First World War.
Note: Gillies work was not confined to those injured in Trench Warfare, his first influx of patients was a group of men badly disfigured during the Battle of Jutland.
Treating Shellshock
Shellshock is a psychological condition suffered by many of the men who fought in the First World War. At first it was defined by the soldiers proximity to bombardments, giving it the name shellshock. Later in the war the understanding of mental trauma caused by the conflict had broadened. It became recognised that any experiences of war could lead to mental trauma. These traumas exhibited themselves in a wide range of ways. President of the British Psycho-Analytic Association, Ernest Jones, explained:
…to indulge in behaviour of a kind that is throughout abhorrent to the civilised mind…. All sorts of previously forbidden and hidden impulses, cruel, sadistic, murderous and so on, are stirred to greater activity, and the old intrapsychical conflicts which, according to Freud, are the essential cause of all neurotic disorders, and which had been dealt with before by means of ‘repression’ of one side of the conflict are now reinforced, and the person is compelled to deal with them afresh under totally different circumstances
Shellshock came to be a huge problem for the army. 80% of those suffering from it were unable to return to active service during the First World War. Men suffering from the condition were identified as having either a nervous condition or a psychological one. Nervous conditions could be treated by massage, diet, electric shock treatments. Psychological cases were more difficult. There was an onus on retaining the masculinity of the men, so facing up to the things that they had seen, done or heard were very much the order of the day. Talking treatment encouraged them to face his illness in a manly way.
Shellshocked men also faced public stigmatisation. Even in hospitals they were frowned upon. Siegfried Sasoon wrote the poem Survivors about his experiences of shellshock:
No doubt they’ll soon get well; the shock and strain
Have caused their stammering, disconnected talk.
Of course they’re ‘longing to go out again’, –
These boys with old, scared faces, learning to walk.
They’ll soon forget their haunted nights; their cowed
Subjection to the ghosts of friends who died,
Their dreams that drip with murder; and they’ll be proud
Of glorious war that shatter’d their pride…
Men who went out to battle, grim and glad;
Children, with eyes that hate you, broken and mad.
Gas attacks: how were victims treated?
Medicine in the First World War had to deal with the new problem of Gas attacks. Though prevention through the use of gas masks was attempted, many men suffered the affects of gas attacks. Gases used in the war caused a number of medical issues. Inhaled, they could choke a man by filling his lungs with the gas and in effect drowning him. Some of the gases used caused blistering. This could be internal as well as external. Gas could impact on the soldiers vision, leading to blindness in the most severe cases. Medics could potentially be faced by a soldier suffering from any combination of these complaints. The range could be from superficial injuries to third degree burns, blindness, suffocation.
Casualty figures for British Troops show that gas accounted for 1% of the 750,000 men who died. However, it caused 180,100 wounded. A sizeable number of men. Only 20% of these men were able to return to the front lines.
The early response of the British Medical Teams to gas attacks and wounds caused by them was to send the men for long periods of recovery at Base Camps, or to send them to convalesce back in Britain. To a large extent this was because they didn’t have a fully effective treatment of the conditions they saw. Time was a healer in such cases. As the war progressed studies of the physiological and psychological impact of gas were conducted. This led to changes in treatment being made by British Medical Staff in 1917. From this point onward specialist teams were deployed close to the front lines to tackle the affects of gas. Some of the ideas were taken from studies of men who had been shell shocked: the panic caused by being gassed was a serious concern in itself.
Dulce et Decorum Est, a War Poem by Wilfred Owen, relates to Gas Attacks. It highlights the psychological impact of hearing the thud of a gas shell landing in this section:
Gas! GAS! Quick, boys!—An ecstasy of fumblingFitting the clumsy helmets just in time,But someone still was yelling out and stumblingAnd flound’ring like a man in fire or lime.—Dim through the misty panes and thick green light,As under a green sea, I saw him drowning.In all my dreams before my helpless sight,He plunges at me, guttering, choking, drowning.

Gas was not necessarily intended to kill. It’s psychological affect was huge. In some cases cans of fresh air were fired to terrify the enemy, on at least one occasion designed to lull them into believing that all shells would be fake. An account after the first British use of Gas noted:
A German officer in this sector remarked that as soon as the gas entered his trench, he lost all control of his men, a panic ensued and he was unable to keep them in the front line. He said that, without the gas, we should have had no earthly chance of taking the trenches
Diagnosis and Treatment:
Step 1: Identify the patient as having been gassed, done by using a crayon to mark their forehead.
Step 2: Determine extent of the injury. This was difficult as sometimes the injury was psychological, men fearing they had suffered from gas. If actual, was it acute?
Step 3: Decontaminate and ensure other soldiers and the medical staff are not in contact.
Treatments varied:
Burns: the patient was washed and a sodium hypochlorite skin soaking applied. Burns from gases such as Mustard Gas could continue to blister for some time and were up to third degree burns.
Eyes: irrigation (water) was commonly used. For more acute cases atropine ointment could be used. This eased spasms of the eyelids and dilated the pupils artificially. Treatment could last several weeks.
Inhaled gas: the inhalation of gas could lead to blistering and ulcers. This made it difficult for patients to breathe. Treatment was rest and oxygen was used to ease breathing.
Mustard Gas: the US Army had mobile shower units that were designed specifically for hosing down men who may have come into contact with mustard gas.
X-Ray’s on the front lines
Surgeons benefit from having a clear understanding of the nature of internal wounds. Broken bones are best fixed where the nature of the break is known. X-Rays were able to produce rudimentary imaging of broken bones etc by the time of the First World War, having been invented by William Roentgen in 1895. The problem for surgeons was that the X Ray machines were in large hospitals in Paris and the urgent medical need was at Base Hospitals near the front lines.

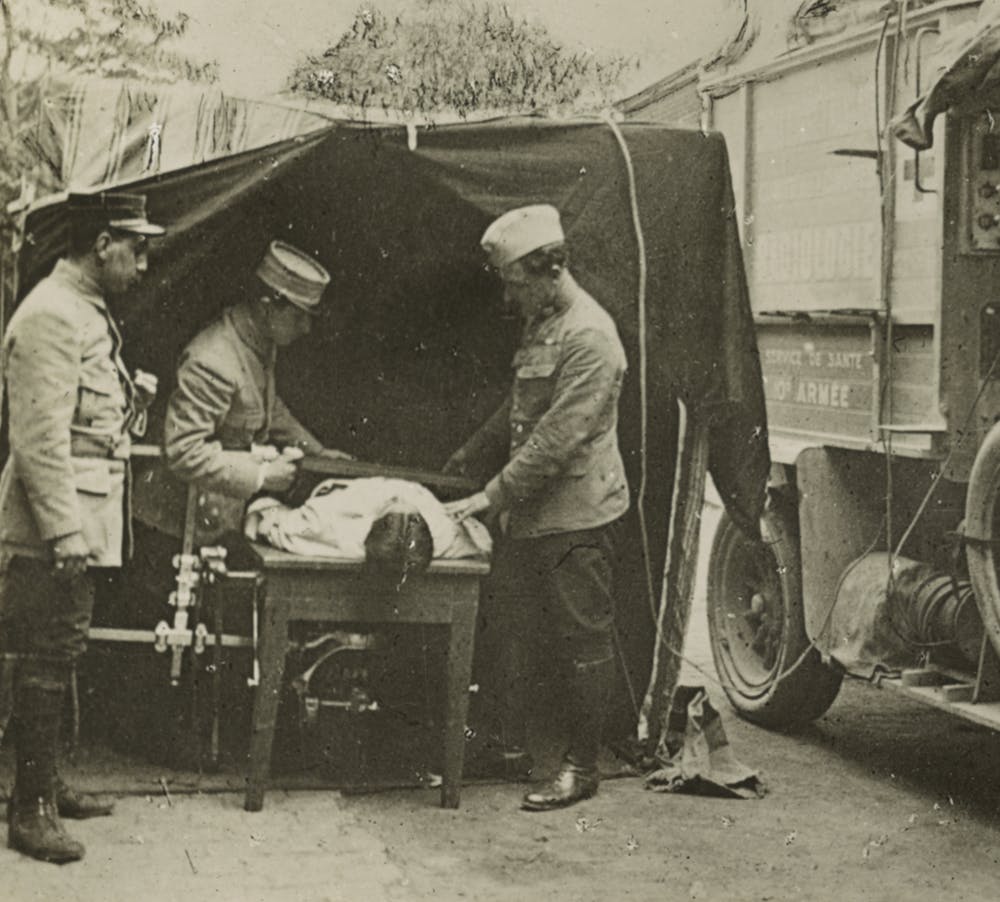
Step forward double Nobel Prize Winning scientist Marie Curie. Curie had sent her scientific research into safety in Bordeaux as the Germans advanced on Paris. Noting the problems faced by doctors and the lack of available X-Rays, an area in which she was interested, she set about tackling the problem. Curie devised a mobile X-Ray ambulance. An X-Ray Machine was built into the bay to the rear. A Dynamo was fixed to the vehicle to collect a battery charge as the ambulance moved. The charge could then be used to power an X-Ray machine.
150 women were trained in the use of these mobile X-Ray Ambulances. These were able to drive to Base Hospitals based on priority areas.
Not content with ‘just’ inventing the first mobile medical imaging vehicle, Curie then organised the construction of 200 X Ray bays at Field Hospitals along the front lines.
Thanks to Marie Curie’s innovation military medicine has been making use of mobile X Ray (and other imaging at later dates) ever since. This allows rapid diagnosis which improves the quality of treatment.
Link: The Smithsonian Magazine has a good article on Marie Curie and the mobile X Ray Ambulance.
Field hospitals
Footage of a First World War Field Hospital
Hospital Ships and Hospitals in Britain
The number of wounded men during the First World War led to non medical buildings and ships being converted into makeshift hospitals. These included ships that held thousands of wounded men and stately homes that opened up their rooms to nursing of injured men.

Blood Transfusions
The concept of Blood Transfusions had been around for some time. Since William Harvey’s work on the Circulation of Blood there had been attempts to transfer blood from one person to another. Most had disastrous effects. It was not until 1900 that Karl Landsteiner identified different blood groups. This meant that it was now easier to transfer blood without it having the risk of contamination, rejection and complications. However, in 1914 the process of transfusing Blood was incredibly difficult. A surgeon faced the problem of Blood clotting as it was transfused. This could prove fatal.
As war was breaking out it was discovered that sodium citrate could be used as an anticoagulant. This thinned the blood and reduced the risk of it clogging. It wasn’t especially reliable though, it was an improvement but far from ideal. In 1916 a new anticoagulant, Heparin, was discovered by Jay Maclean. Heparin is a highly efficient anticoagulant. It is still used today. Its introduction into battlefield medicine was a major development.
Important note: The anticoagulant properties of Heparin were discovered in the United States before they entered the war.

The use of Heparin and effective Blood Transfusions on the Western Front took place after the USA entered the war in 1917. Captain Oswald Hope Robinson of the US Army devised a system of blood banks and transfusions. He revolutionised the way that the process took place. Prior to his work blood had been transfused almost as soon as it had been taken from a donor. Robinson devised the concept of the Blood Bank. This collected and stored a large amount of blood of each type. As a result it was available to surgeons as and when required. Donor systems were also set up.
The Blood Donor system and Blood Banks are still in use in Britain today. They are a direct result of Robinson’s system. Robinson’s system was made possible by the discovery of Heparin’s properties and Landsteiner’s earlier discovery of Blood groups.
A Battlefield Surgeons Equipment

Surgical Equipment available to Battlefield hospital surgeons was little different to that available for surgeons in established hospitals. The constraint would be that the equipment needed to be mobile, so would be selected to fit into cases such as the one above. Surgeons tools includes forceps to hold wounds open, saws to cut through bone and sinew, drills which would be used to drill into bone to enable plates to be fixed.

Trench Foot
One of the best known ailments of the First Wold War is Trench Foot. Men wore boots for long periods of time. Often the conditions were waterlogged. The two combine to create very poor conditions for foot hygiene. This sometimes resulted in soldiers feet becoming so badly infected that toes had to be amputated. The army needed to keep men’s feet healthy. Afterall, a soldier needs feet to march or run in combat. Treatments for Trench Foot included powers such as the one below.

Links
Medicine Through Time – The First World War – Technology and war – War as a factor in the History of Medicine